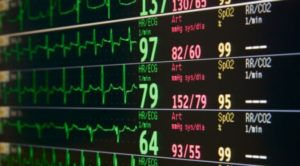
Maria Cvach, DNP, RN, FAAN, who is director of policy management and integration for Johns Hopkins Health System, recently spoke with the Physician-Patient Alliance for Health & Safety (PPAHS) about the experience of John Hopkins Hospital in improving patient safety and reducing alarm fatigue.
Clinical Education Podcast Features Maria Cvach on Reducing Alarm Fatigue
In a clinical education podcast that was released on PPAHS’s YouTube Channel, Ms. Cvach discussed how John Hopkins Hospital was ahead of the curve in managing alarm fatigue, which became The Joint Commission proclaimed as a national patient safety goal in 2014. Johns Hopkins Hospital had formed an alarm management committee in 2006:
Continue reading “Maria Cvach’s 6 Steps for Improving Alarm Management”